A sweeping federal budget law is quietly threatening the health coverage of some of America’s…
Suicide Among the Elderly Going Up
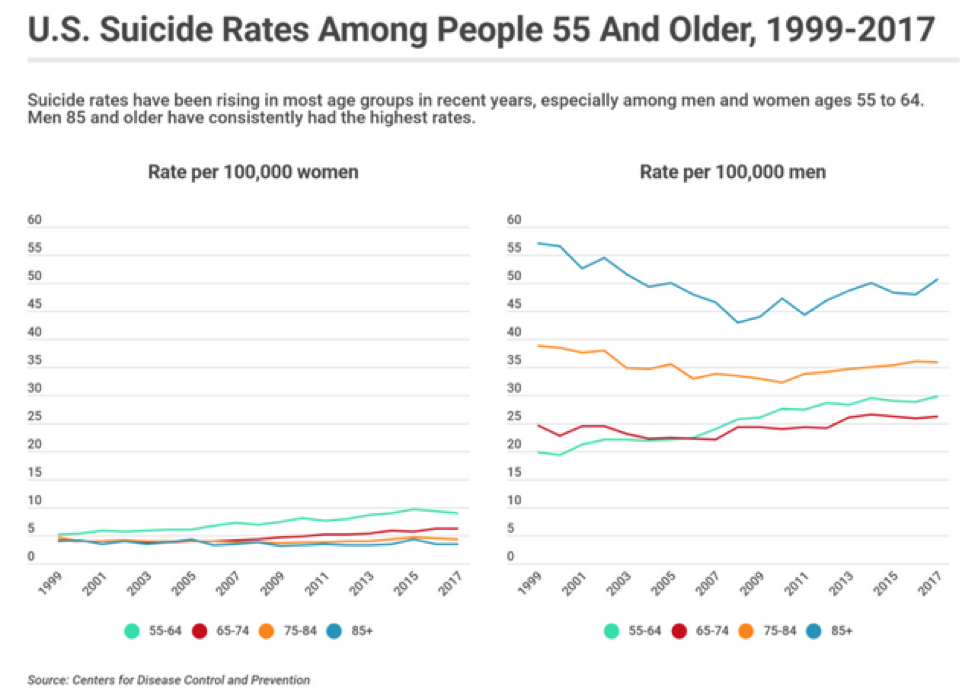
An increasing number of older Americans are turning to suicide particularly when they live in long term care facilities, assisted living, and continuing care retirement communities. Experts agree that this late-life suicide trend is generally under-recognized, under-documented, and poised to grow. The highest rates are among men aged 85 and older, and according to the Center for Disease Control and Prevention (CDC), 54 percent of those elder Americans who commit suicide do not have any known mental health conditions. Suicide attempts by the elderly are likely to result in death as older adults: plan carefully, use more deadly methods, and are less likely to be discovered or “rescued,” and less likely to recover from an unsuccessful attempt due to their physical frailty.
Certain life events and conditions can bring about despair so profound that a senior opts to take their own life. Generally, it is a combination of factors rather than a single problem that instigates suicidal thoughts, planning, and the actual suicide event. These wide-ranging factors include relationship issues, substance abuse, physical health challenges, life crisis events, financial or employment factors, housing-related issues, and legal issues.
While many cultures celebrate the aging process and show deep respect to their elders, in Western cultures like the United States the elderly are typically removed from their community and “outsourced” to nursing homes, long term care, or assisted living facilities as their children are unable or unwilling to provide caregiving assistance. Even those younger family members who do provide nurturing care for their aging parents can miss the signs that are linked to suicide. Some aging Americans feel they are marginalized and a burden to their family system.
Learn the signs of suicide risk and how best to prevent it if your parent or a loved one is living in, or soon to transition to, a long term care living situation. Look for the 4 “D’s” which include: depression, disability, access to deadly means, and disconnectedness. A new environment (aka not “home”) can create anxiety and insomnia leading to muscle aches, headaches, changes in appetite and weight, or an increase in agitation. Know what is normal for your parent and if you see a change in them do not be afraid to ask about it. Inquire about what makes them look forward to the day; the types of activities and social interactions they find that best suits their preferences. Ask what they like about where they are living and also what they don’t like about it. Listen carefully. If there is a significant enough problem, let the staff know and try to get the issue corrected. If your loved one relates to you that they want to die or share suicidal thoughts with you alert the caregiving staff immediately. Know what the suicide protocols are in the facility and be able to differentiate between actively and passively suicidal.
Losing a parent or loved one to the increasing trend of senior suicide is devastating to a family, as is wondering what was it that put them in such a desperate place to take their own life.
Below are additional resources to share with loved ones. If we can be of further assistance, please don’t hesitate to reach out. You can reach the Estate Planning & Elder Law Center of Brevard by clicking here to send us a message or by dialing us at (321) 729-0087.
Resources:
The National Suicide Prevention Lifeline at 1-800-273-8255, or use the online Lifeline Crisis Chat, both available 24 hours a day, seven days a week.
People 60 and older can call the Institute on Aging’s 24-hour, toll-free Friendship Line at 800-971-0016. IOA also makes ongoing outreach calls to lonely older adults.